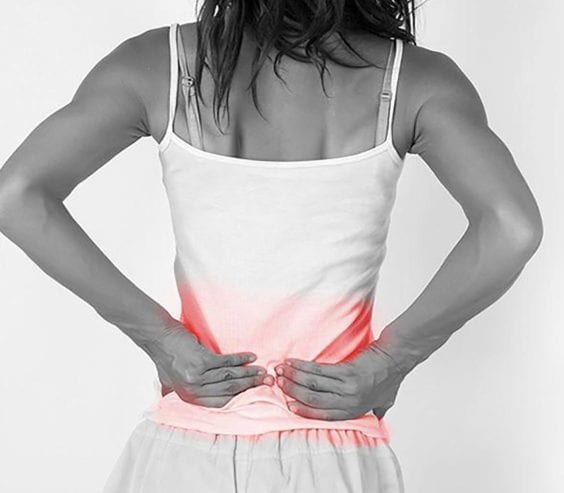
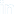Degenerative disc disease and the resulting low back pain are the most among the most common complaints by patients to their healthcare providers. An estimated 80% of the population will suffer back pain at some point in their life. Without the proper diagnosis, a difficult road can lie ahead for those caught in the grips of low back pain. A simple way to get an idea of how serious your back or degenerative disc disease may be is to complete this 3-minute Back Pain Score and get your result today. Ultimately, the pain can rob one of quality of life and your best option is often an evaluation with an Oklahoma Pain Specialist.
In an effort to prepare patients for combating low back pain, we provide here a summary of five of the most common causes of lower back pain.
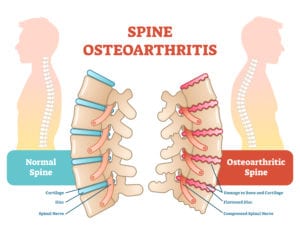 Arthritis of the Spine
Arthritis of the Spine
Arthritis is among the most common causes of low back pain and increases in frequency as we age. Symptoms include recurrent back tenderness, soreness, morning stiffness, and difficulty carrying out tasks of daily living such as sweeping or vacuuming. The most common specific type is osteoarthritis of the spine.
As part of the natural process of aging, the spinal column is susceptible to the constant pull of gravity and the repetitive nature of our daily tasks. Conditions including spondylosis, facet arthropathy, and osteophyte formation are characteristic features of the aging spine. In addition, a history of significant spinal trauma such as in motor vehicle accidents and contact sports injuries commonly contribute to the premature advancement of spine arthritis.
Ultimately, increasing pain levels, spinal stiffness, loss of flexibility, and reduction of mobility are some of the reasons patients should seek interventional pain specialist care.
Degenerative Disc Disease
The discs in our spine act as shock absorbers between the spinal bones in our back known as vertebrae. The spine of the low back is made up of 5 distinct vertebral bones and 5 associated discs between the 1st and 2nd bones, 2nd and 3rd bones, 3rd and 4th bones, 4th and 5th bones, and 5th bone and the sacrum. Over time and with injuries to the back, the discs can lose water content, nutrients, and become less flexible. As this happens, the discs will shrink, which often contributes to the loss of height experienced by most people as we age. Ultimately, degenerated vertebral discs can result in chronic pain in the back that can become significant and even debilitating. Degenerated discs also are more likely to suffer further injury that could lead to disc bulging, disc protrusion, and/or disc herniation. The natural process of wear and tear eventually shows up in everyone’s spine however, early onset or severe degenerative disc disease can result in the need to seek medical care from a pain specialist.
Associated conditions seen in conjunction with degenerative disc disease include spine arthritis, spondylosis, radiculopathy, annular tears, facet joint arthritis, facet hypertrophy, muscle spasm, lumbago, sciatica, and sciatic nerve pain.
Initial treatment of degenerative disc disease commonly includes conservative approaches such as anti-inflammatory medications, physical therapy, and chiropractic care. Should these therapies fail to appropriately relief the associated back pain, an evaluation with a pain specialist should be performed. Therapies such as epidural injections, spinal cord stimulation, spine interventions, and radiofrequency ablation may provide substantial relief following a back pain doctor’s diagnosis. Only as a last resort would spine surgery be considered given the risks involved.
Herniated And Bulging Discs
As described previously, vertebral discs act as the cushioning between back bones (vertebrae). When the outer layer of a disc becomes weakened or torn, the inner jelly-like portion of the disc can bulge or protrude (herniate) outside the normal area of a disc. When this happens, the spinal cord or spinal nerve roots can become mechanically compressed which can result in what many refer to as a “pinched nerve” in the back. This can be very painful and results in millions of patients having severe back and even associated leg pains (sciatica, radicular pain). There is also a chemical effect when the disc is ruptured resulting in substances leaking out of the disc and irritating the surrounding nerves.
Bulging discs are extremely common and depending on the size, position, and other factors, they may or may not be the root cause of your pain. A herniated disc more often does cause pain and more significant levels of herniation can result in associated weakness as well. A spine pain specialist is uniquely suited to identify whether your bulging or herniated discs are the primary cause of your painful low back symptoms.
Spinal Stenosis
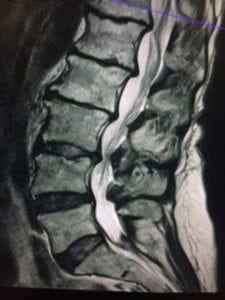
Spinal stenosis is defined as an abnormal narrowing of the vertical channel formed by the vertebral backbones that protect the spinal cord. Stenosis within the spine often occurs as a result of spinal arthritis, degenerative disc disease, herniation of disc material into the spinal canal, or some combination of these.
Another potential cause is known as spondylolisthesis, which occurs when a vertebral bone slips forward and out of place relative to an adjacent vertebral bone. The result can be a significant narrowing within the spinal canal due to the lack of alignment of the spinal column.
An associated condition, referred to as neuroforaminal stenosis, occurs when the side openings formed by two adjacent vertebrae (backbones) become crowded with material. These side, or lateral openings, allow the passage of nerve roots branching fr
om the spinal cord to reach their target sites and these nerves are vulnerable as they pass through the small openings between the backbones. When the nerve roots become compressed, the result is often pain, numbness, tingling, and this may progress to weakness of the foot or leg.This is most often seen with degenerative disc disease because the loss of disc height contributes to the closing of the side openings on the spine.
Proper evaluation and treatment by a spine pain specialist is highly recommended should you suffer spinal stenosis or neuroforaminal stenosis. Non-surgical treatments options include transforaminal epidural, interlaminar epidural, caudal epidural, and spinal cord stimulation. The best treatment for your specific condition can be recommended by your Interventional Pain Management Specialist.
Muscle Spasms, Trigger Points, & Muscle Strain
Muscle spasms are extremely common and very often associated with underlying spinal joint, spinal disc, or spinal stenosis related disease or injury. Think of muscle spasms as our body’s reflex reaction to most spine related injury or pain. Most often, when the underlying spinal problem is appropriately treated, muscle spasms tend to improve. However, the muscular soft tissue may require specific rehabilitation at the direction of your spine pain specialist.
Trigger points are simply discreet regions of muscle that is undergoing localized spasm and inflammation. They usually develop as a result of chronic stress and irritation to certain muscle groups and nerve roots of the spine. These areas within the muscle are often felt as small to medium sized lumps under the skin that are frequently tender to the touch.
Muscle strain or “pulled” muscles may result from the overuse of a muscle or group of muscles. This can also occur with vigorous physical activity, repetitive use injuries, or trauma (car accidents, sports injuries, etc.).
Muscle spasms and trigger points are often treated with muscle relaxants, anti-inflammatory medication, physical therapy, physiotherapy, manipulation, trigger point injections, TENS therapy, acupuncture, and nerve block injections. An Interventional Pain Specialist has the expertise to identify the most appropriate course of treatment and often will use more than one technique to achieve the desired improvement of your low back pain.
Conclusion
Whether osteoarthritis, degenerative disc disease, herniated discs, bulging discs, spinal stenosis, muscle spasms, or trigger points, the best choice for evaluation and treatment of your low back pain is often an Interventional Pain Specialist. Once you have a properly diagnosed pain condition, the best treatments can be provided. As a sub-specialty trained pain treatment doctor, we have the unique skills required for the most effective low back pain relief without surgery. If you or someone you know is suffering from the debilitating nature of low back pain, relief is within reach. We look forward to getting you back to the life you deserve.

 CALL TODAY!
CALL TODAY!